Some people in Euless or Dallas know they need more than a weekly therapy appointment, but the idea of stepping away from work, parenting, school, or daily responsibilities feels impossible. A person may be holding a job during the day, trying to manage cravings at night, and telling family members that things are “fine” when they clearly are not.
That tension is real. Many adults are not avoiding treatment because they do not care. They are trying to survive while keeping life from falling apart.
Consequently, many people first ask, what is IOP therapy? They are not looking for a technical definition. They are looking for a treatment option that is strong enough to help, but flexible enough to fit everyday life.
An Intensive Outpatient Program, or IOP, is often that middle ground. It gives people a structured level of care without requiring them to live at a facility. That matters for the person who still needs to clock in, pick up children, attend class, or sleep in their own bed while getting help for substance use, mental health concerns, or both.
For families, IOP can also bring relief. It creates a plan. Instead of relying on promises, guesswork, or constant crisis management, treatment becomes consistent and visible. Sessions are scheduled. goals are tracked. Skills are practiced in practical situations, not just talked about in theory.
In the Dallas-Fort Worth area, this level of care often fits adults who need meaningful support but do not need round-the-clock supervision. It can also be a strong option for people dealing with opioid use and co-occurring depression, anxiety, or trauma who need treatment that includes therapy and medication support.
Table of Contents
- Introduction Finding Hope When Life Cant Stop for Treatment
- What Exactly Is Intensive Outpatient Program Therapy
- IOP Compared to Other Levels of Addiction Treatment
- A Typical Week in an IOP Program in Euless TX
- Integrating Dual Diagnosis and MAT with IOP Therapy
- Is an IOP in the Dallas Area the Right Fit for You
- How to Start IOP at Maverick Behavioral Health
- Common Questions About IOP Therapy
Introduction Finding Hope When Life Cant Stop for Treatment
A working parent in Dallas may wake up already overwhelmed. There is a commute to manage, messages from school, bills to pay, and a growing dependence on alcohol, pain pills, or another substance that no longer feels manageable. By evening, the same person may be frightened by how much control has been lost, but still believe treatment would require disappearing from daily life.
That belief keeps many people stuck.
IOP therapy exists for this exact kind of situation. It is not a watered-down version of care. It is structured treatment built for people who need serious help and still have life obligations waiting for them at home.
Why this level of care matters
The word intensive can sound intimidating. The word outpatient can sound too light. Together, they describe something practical. A person receives meaningful treatment several times each week, then returns home and keeps practicing recovery in ordinary life.
This creates a bridge between two extremes:
- Weekly therapy alone may not provide enough structure for someone in active struggle.
- Residential care may be more support than a person needs, or more than their schedule can realistically accommodate.
For many adults, IOP sits in the middle.
Key takeaway: IOP therapy is designed for people who need more than occasional support, but who can still live safely at home and participate in treatment consistently.
Where people often feel confused
Families sometimes assume outpatient means low commitment. It does not. IOP asks for time, honesty, and active participation.
Others assume treatment only works if someone leaves normal life behind. In many cases, the opposite can be true. When a person learns skills in treatment and uses them that same day at work, at home, or during stressful moments, recovery becomes more grounded and more realistic.
For people across Euless, Dallas, and the broader DFW area, that is often the first hopeful shift. Treatment does not have to mean pressing pause on everything. It can mean finally getting the right level of support while life keeps moving.
What Exactly Is Intensive Outpatient Program Therapy
What is IOP therapy? In simple terms, it is a structured treatment program that provides several hours of care each week while allowing the person to live at home.
A useful comparison is school. Residential treatment is closer to living on campus full time. IOP is more like taking a demanding course load while still living at home and keeping up with the rest of life. The work is serious. The schedule is organized. The support is consistent. But the person returns home after each treatment day.
What makes it intensive
IOPs are classified as ASAM Level 2 care and provide 9 to 15 or more hours of structured treatment per week, often in 3-hour sessions held 3 to 5 days weekly, while allowing people to live at home and maintain work or school commitments, according to American Addiction Centers’ overview of intensive outpatient programs.
That schedule gives treatment enough repetition to build momentum. A person is not waiting an entire week between sessions to address relapse triggers, emotional crashes, or family stress.
What happens in treatment
Most IOPs use a mix of therapies rather than relying on one conversation format.
Common elements include:
- Cognitive Behavioral Therapy or CBT helps people identify thought patterns, triggers, and behaviors that fuel substance use or emotional distress.
- Dialectical Behavior Therapy or DBT teaches emotional regulation, distress tolerance, and healthier ways to respond when feelings become intense.
- Motivational Interviewing helps people work through ambivalence. This matters when part of a person wants change and another part still resists it.
- Group therapy creates accountability, perspective, and support from others facing similar challenges.
- Individual counseling gives space for more personal treatment planning and deeper work.
- Complementary supports may include mindfulness or yoga. IOPs often use these alongside CBT and DBT to strengthen emotional regulation and reduce stress, especially for people with co-occurring disorders, as noted in this summary of data-informed IOP approaches.
The philosophy behind IOP
IOP is not just about attending sessions. It is about learning a skill on Tuesday and needing it on Tuesday night.
A person may discuss cravings in group, practice a coping strategy in session, and then use that same strategy after a difficult phone call or during the drive home. That direct link between treatment and daily life is one reason many people find IOP both challenging and effective.
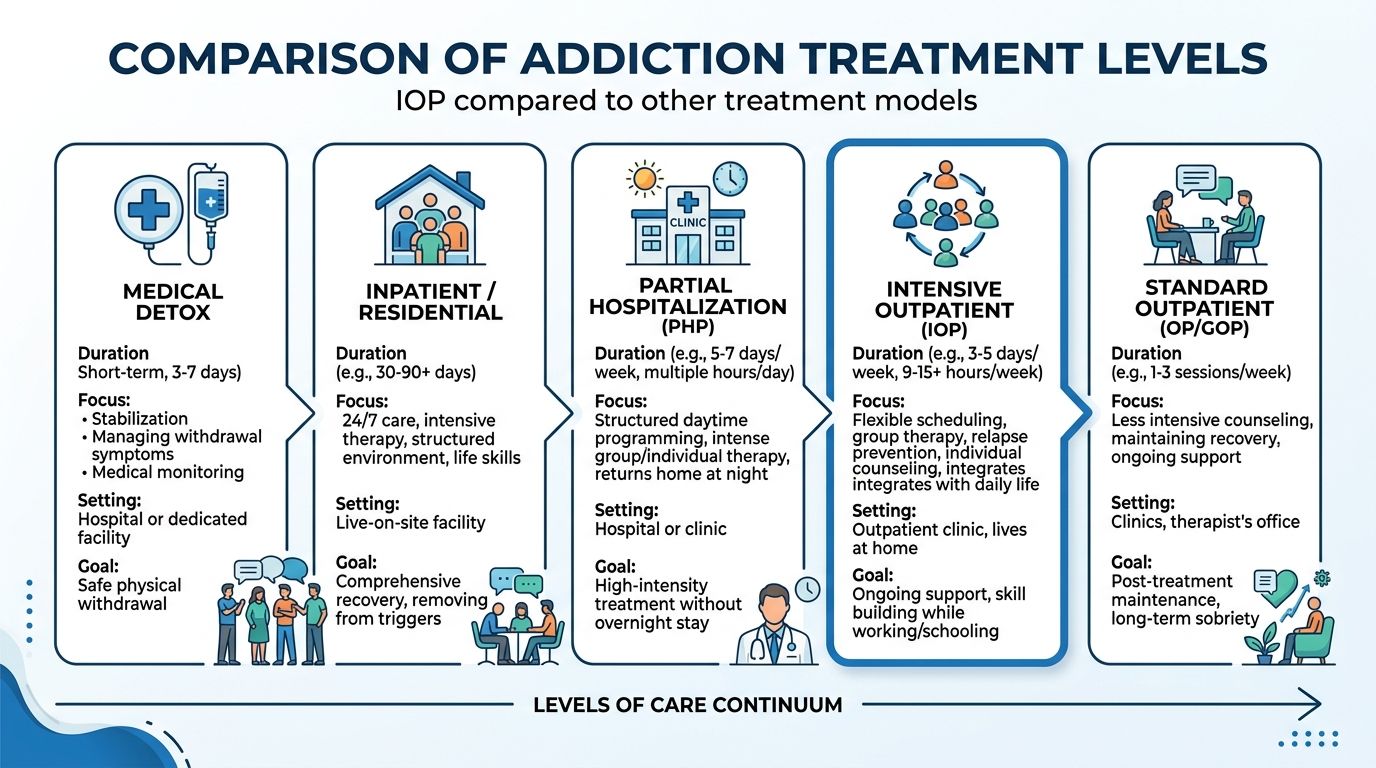
IOP Compared to Other Levels of Addiction Treatment
A common point of confusion for families is whether treatment has to be either weekly therapy or a full residential stay. In practice, addiction care works more like a ladder. Each level adds more structure, support, and clinical oversight based on what the person needs right now.
IOP often sits in the middle of that ladder. It gives people more contact than standard outpatient care, while still leaving room for work, family life, and daily responsibilities. For a working professional in Euless or Dallas who is trying to protect a job, manage childcare, or keep up with bills, that middle ground can matter a great deal.
The practical difference
Standard outpatient care usually works best for someone whose symptoms are fairly stable. They may need therapy, relapse prevention support, or medication follow-up, but they can function safely with less frequent contact.
IOP adds a stronger frame around the week. A person attends treatment several days each week, stays connected to clinicians and peers, and practices recovery skills while still living at home. That matters in opioid treatment and dual-diagnosis care, where cravings, mood symptoms, and medication needs often change in real time rather than once a week.
PHP is a step above IOP in intensity. It usually fits people who need most of the day structured around treatment but do not need overnight care. If you are comparing those options, this overview of a partial hospitalization program in Dallas, Dallas County, Texas explains how PHP differs from lower levels of care.
Comparing levels of outpatient care
| Feature | Standard Outpatient | Intensive Outpatient (IOP) | Partial Hospitalization (PHP) |
|---|---|---|---|
| Structure | Lower structure | Moderate to high structure | High structure |
| Weekly commitment | Usually a few appointments | Several treatment sessions across the week | Most weekdays for much of the day |
| Living arrangement | Lives at home | Lives at home | Lives at home |
| Best fit | Stable symptoms and lower relapse risk | Needs strong support while maintaining work, school, or family responsibilities | Needs more daily oversight without overnight stay |
| Common use | Ongoing therapy or step-down support | Middle level of care for addiction and dual diagnosis | Step-down from residential or alternative to inpatient for some clients |
For many adults, the choice is less about which level sounds stronger and more about which level matches the actual risk. Someone using opioids who is starting or continuing Medication-Assisted Treatment may need more than a weekly counseling visit. They may need frequent check-ins, group support, relapse prevention work, and close coordination around medication, all without stepping away from work completely. That is one reason IOP can be such a practical fit.
How to think about the right choice
Three questions usually help clarify the decision.
- How much support is needed between sessions to stay safe and steady?
- Can the person live at home without round-the-clock supervision?
- Would a flexible schedule make it more likely that treatment can continue long enough to help?
IOP works well when weekly therapy is not enough, but a full-day program would be more than the person needs or more than life can reasonably allow. It is often the level where recovery starts to become usable in real life, especially for people balancing opioid recovery, MAT appointments, anxiety or depression treatment, and a job in the Dallas-Fort Worth area.
Practical guide: The right level of care should match the person's current risk, daily responsibilities, and ability to function safely outside a facility.
A Typical Week in an IOP Program in Euless TX
A typical IOP week has to fit real life. For many adults in Euless, Dallas, and nearby communities, that means work during the day, treatment in the evening several times a week, and time at home to practice what was discussed in session.
That schedule matters. Recovery is not happening in a bubble. It is happening before the commute home, after a stressful shift, during family tension, and in the quiet hour when cravings often get louder.
What a session often includes
An IOP session usually has structure and movement. It is not only one long talk with a counselor. Each part serves a purpose, much like a good physical therapy plan combines instruction, practice, and feedback.
A session often includes:
- Group process work where clients discuss cravings, setbacks, progress, work stress, family strain, and patterns that can lead back to substance use.
- Skills-based education focused on relapse prevention, emotional regulation, communication, boundary setting, and coping with high-risk situations.
- Individual check-ins so the clinical team can adjust goals, respond to setbacks early, and coordinate care when someone is also receiving MAT or mental health treatment.
- Family involvement when appropriate to improve communication, reduce enabling patterns, and support recovery at home.
The rhythm is practical. Learn a skill, try it in daily life, come back, and review what happened.
Why living at home matters
One of the strongest parts of IOP is that treatment happens alongside normal life. A person leaves session and returns to the places where recovery has to hold up: home, work, relationships, pharmacies, old triggers, and familiar routines.
Research shows IOP can be effective because people practice coping skills in their everyday environment rather than only in a protected setting. That gives clinicians useful information. If a plan sounds good in group but falls apart after work on Thursday, the team can help revise it before the pattern turns into a relapse.
For working professionals, this often makes IOP more usable than a model that pulls them completely out of their week. Someone can attend treatment, continue MAT appointments, stay connected to family responsibilities, and still get repeated clinical support.
A simple example
Take a working adult in Euless who notices opioid cravings rise around 6 p.m. after a long commute. By the time they get home, they are tired, irritated, and alone for an hour before anyone else arrives.
In IOP, the clinician and group help break that risk pattern into smaller parts. The person may identify fatigue, isolation, access to pills, and the thought that using will bring quick relief. Once those links are clear, the treatment plan gets more specific.
It might include a medication check-in if the person is on MAT, a ride-home call with a support person, a planned meal before cravings peak, a short walk before entering the house, and a script for handling conflict with a partner. Recovery works like building guardrails on a dangerous stretch of road. The goal is not willpower alone. The goal is to make the high-risk hour safer and more predictable.
That is why a typical IOP week can be so effective. Clients are not waiting to use recovery skills someday. They are using them in the exact settings where they need them most.
Integrating Dual Diagnosis and MAT with IOP Therapy
A lot of adults in Euless and Dallas do not walk into treatment with only one problem. They may be trying to stop opioid use while also dealing with panic after work, depression that drains motivation, or trauma symptoms that flare up at night. If care treats those struggles as separate lanes, recovery can feel scattered and frustrating.
Integrated treatment brings those lanes together.
What dual diagnosis means in daily treatment
Dual diagnosis means a person has both a substance use disorder and a mental health condition at the same time. One often intensifies the other. Anxiety can push someone toward opioids for relief. Opioid use can worsen mood, sleep, concentration, and emotional stability.
That is why treatment works better when both conditions are addressed in the same plan, by the same team, with the same goals in view. Someone looking for that type of coordinated care can learn more about dual diagnosis rehab.
A simple way to picture it is this. If a person has a sprained ankle and keeps walking on it, pain medication alone will not fix the injury. In the same way, counseling alone may not be enough if cravings, withdrawal, depression, and trauma symptoms are all feeding each other. Each part needs attention.
How MAT fits into IOP
For opioid use disorder, Medication-Assisted Treatment, or MAT, often includes medications such as Suboxone to reduce cravings and withdrawal. Therapy in IOP then helps the person build the skills that medication cannot provide on its own, such as handling stress, repairing routines, setting boundaries, and responding differently to triggers.
The roles are different, but they work together.
Medication helps steady the body. Therapy helps steady daily life.
For working professionals, that combination often matters in very practical ways. A person who is not fighting constant cravings or feeling sick during the day is more able to focus in group, keep medical appointments, stay present at work, and practice recovery skills at home. SAMHSA has noted in its treatment guidance that medications for opioid use disorder are associated with better treatment engagement and support long-term recovery when paired with counseling and behavioral care.
Why integrated IOP care matters for dual diagnosis
People with opioid use disorder and mental health symptoms often get stuck in a loop. The medication piece may help lower the physical pull to use. The therapy piece helps explain what still happens emotionally after that physical intensity starts to settle.
For example, a professional in the Dallas area may start MAT and notice fewer cravings within days, yet still feel overwhelmed every Sunday night before the workweek starts. That does not mean treatment is failing. It often means the opioid use was only one part of the coping pattern. IOP gives space to work on the other part. The person can examine stress, perfectionism, shame, relationship conflict, or untreated depression that still raises relapse risk even after withdrawal improves.
This is especially important in dual-diagnosis care. Once the nervous system is more stable, therapy can get more precise. Group sessions can focus on relapse triggers. Individual counseling can address trauma or mood symptoms. Medication follow-up can track how the current plan is affecting sleep, focus, cravings, and functioning across the week.
Why this model fits many adults in Euless and Dallas
Adults with jobs, children, or caregiving responsibilities often need treatment that fits real life instead of pausing it completely. An IOP that coordinates MAT and mental health care can support that reality.
It can help by:
- Reducing the day-to-day strain of early recovery. Lower cravings and fewer withdrawal symptoms make it easier to stay engaged.
- Creating one coordinated treatment plan. Therapy, medication support, and mental health care are aligned instead of disconnected.
- Making room for dual-diagnosis work. Once physical symptoms settle, treatment can focus more clearly on anxiety, trauma, depression, and relapse patterns.
- Supporting consistency for working adults. Structured care can happen while a person continues work and family responsibilities.
At Maverick Behavioral Health, we often explain MAT and IOP as two hands doing different jobs at the same time. One helps stabilize the brain and body. The other helps the person rebuild judgment, routines, relationships, and confidence. For many adults recovering from opioid use while managing depression, anxiety, or trauma, that combined approach gives treatment a better chance to hold under real-world pressure.
Is an IOP in the Dallas Area the Right Fit for You
A common situation looks like this. Someone in Euless or Dallas knows they need more than a weekly therapy appointment, but they cannot disappear from work for a month, stop caring for children, or leave home for residential treatment. They may also be trying to stay on buprenorphine or another medication plan for opioid use while managing anxiety, depression, or trauma symptoms.
In that situation, the primary question is not whether treatment matters. It is whether outpatient treatment offers enough structure to help the person stay safe, consistent, and engaged in recovery while life keeps moving.
An IOP often fits people who need several contacts each week, clear accountability, and coordinated care, but who can still function outside of treatment hours. It sits in the middle ground between once-a-week support and a full-day or live-in program. For many working adults, that middle ground is where treatment becomes realistic.
Signs IOP may be a good match
IOP may be a strong option when the person can benefit from intensive care without 24-hour supervision. That often includes people who are stable enough to sleep at home, go to work, and return for scheduled treatment, but who still need more support than standard outpatient counseling can provide.
A person may be a good fit if several of these are true:
- Home offers enough stability for recovery work. It does not need to be calm or perfect, but it should be safe enough to return to after sessions.
- Daily responsibilities cannot be put on hold. Work, parenting, school, or caregiving still need attention, and treatment has to fit around them.
- The person is able to attend consistently. IOP works best when someone shows up, practices skills between sessions, and stays connected to the treatment plan.
- Withdrawal does not require medical detox. If withdrawal could become dangerous, detox or another medical setting usually needs to come first.
- Symptoms are interfering with daily life. Cravings, relapse risk, anxiety, depression, or emotional swings are strong enough that weekly therapy alone is not enough.
- Medication support needs regular coordination. For opioid recovery or dual-diagnosis care, the person may need therapy, medication check-ins, and mental health treatment working from the same plan.
That last point matters for many adults in the Dallas-Fort Worth area. If someone is using MAT for opioid use disorder, IOP can give the medication a structure to work inside. Medication can help reduce cravings and withdrawal. The IOP schedule helps the person rebuild routines, respond to stress without using, and address the mental health patterns that often drive relapse.
When a higher level of care may be better
IOP is not the right starting point for everyone.
A higher level of care may make more sense if a person cannot stay safe outside treatment hours, has severe or unpredictable withdrawal symptoms, is returning repeatedly to use without any stable support at home, or has psychiatric symptoms that need closer monitoring. In those cases, PHP, residential treatment, or medically supervised detox can create more protection and more observation at the beginning.
Families often worry that choosing a higher level of care means the situation is hopeless. It does not. It means the treatment plan is matching the severity of the problem, the same way a broken bone sometimes needs a cast before physical therapy can help.
What successful participation tends to look like
Good IOP participation usually looks steady, not perfect.
People make progress when they attend sessions regularly, speak openly about setbacks, stay in contact about medication concerns, and use what they learn in real situations at home, at work, and in relationships. For a person balancing opioid recovery with depression or anxiety, success may include taking medication as prescribed, noticing warning signs earlier, and asking for help before a lapse turns into a full relapse.
For adults in Dallas-Fort Worth, the decision often comes down to a few practical questions. Can the person remain safe at home between sessions? Can they commit to treatment several times each week? Will they benefit from care that addresses substance use, mental health symptoms, and, when appropriate, MAT in one coordinated plan?
If the answer is yes, an IOP may be the right fit.
How to Start IOP at Maverick Behavioral Health
Starting treatment feels easier when the process is clear. Individuals generally do not need more pressure. They need a few simple next steps.
Step one is the phone call
A confidential call allows the admissions team to hear what is happening right now. That may include substance use, mental health symptoms, recent relapse, opioid dependence, or concerns about balancing treatment with work.
The call is also where practical questions can be answered, including scheduling and whether IOP or another level of care appears more appropriate.
Insurance and assessment
Many people worry that treatment will be hard to access or impossible to manage. In many outpatient settings, insurance verification is part of the intake process, and most PPO plans are commonly reviewed for eligibility.
The clinical assessment then helps determine what level of support makes sense. That assessment looks at substance use patterns, mental health needs, relapse risk, home stability, and whether services such as MAT should be part of the plan.
A realistic next move
For people specifically looking into opioid recovery options, this overview of opioid addiction treatment near me may help clarify what coordinated outpatient care can involve.
Maverick Behavioral Health provides outpatient substance use and mental health treatment in the Euless and Dallas-Fort Worth area, including IOP, dual diagnosis care, and MAT services such as Suboxone within an individualized treatment plan.
The next step can be small. To talk through options confidentially, call (888) 385-2051.
Common Questions About IOP Therapy
Some questions come up at the very end, after a person already suspects they need help. Those questions matter because they often determine whether someone reaches out or waits longer.
Frequently asked questions
| Question | Answer |
|---|---|
| Will people know someone is in IOP? | Treatment programs are designed to protect confidentiality. The details of participation are handled privately, and staff can explain what that looks like during admissions. |
| Can someone work while attending IOP? | In many cases, yes. IOP is built for people who need structured care while continuing daily responsibilities. Scheduling options often make that possible. |
| Is IOP only for addiction? | No. IOP can support substance use treatment, mental health treatment, or both when a person has co-occurring needs. |
| What if a person needs medication support for opioid use? | Some outpatient programs can integrate MAT, including medications such as Suboxone, with therapy and recovery planning. |
| What happens after IOP ends? | Many people continue with step-down outpatient care, ongoing therapy, medication management, support groups, or aftercare planning to maintain progress. |
A person does not need to have every answer before making the first call. They only need enough willingness to ask for help.
Recovery does not require putting life on hold forever. It requires the right level of support at the right time. For adults and families seeking outpatient addiction and mental health treatment in Euless and the Dallas-Fort Worth area, Maverick Behavioral Health offers a place to start that process with clarity and compassion. To speak confidentially about IOP, dual diagnosis care, or MAT options, call (888) 385-2051.