A person in Dallas-Fort Worth may already know something has to change. Work is slipping. Family members are worried. Promises to cut back keep breaking. At the same time, the idea of disappearing into treatment can feel impossible when rent is due, children need rides, and a job still expects attendance on Monday.
That's where confusion often starts. Many people assume rehab only means living away from home full time. They worry treatment will require pressing pause on everything at once, so they delay the call, even when the situation is getting harder to manage.
What is outpatient drug rehab? It's addiction treatment that lets a person live at home while attending scheduled clinical care during the week. That care can include therapy, group counseling, medication support, and mental health treatment. For many adults in Euless, Dallas, and the surrounding DFW area, outpatient care offers a practical way to begin recovery without stepping away from every responsibility at once.
Outpatient care also isn't a fringe option. It is offered by over 82% of U.S. treatment facilities, making it the most common form of addiction treatment, according to outpatient rehab success and availability data.
Table of Contents
- Real Life Does Not Pause for Recovery
- Understanding the Levels of Outpatient Care
- What a Week in Outpatient Rehab Looks Like
- Outpatient Versus Inpatient The Right Choice for You
- How to Choose a Quality Program in Dallas-Fort Worth
- Begin Your Recovery in Euless with Maverick Behavioral Health
- Frequently Asked Questions About Outpatient Rehab
Real Life Does Not Pause for Recovery
A common story sounds like this. Someone wakes up after another rough night and finally admits the drug or alcohol use isn't under control. Then the next thought hits immediately: “How can treatment happen when there's work at 8, school pickup at 3, and a family depending on me?”
That fear is real. Many adults aren't resisting help because they don't care. They're trying to figure out how recovery fits into an already overloaded life.
Outpatient rehab exists for that exact problem. Instead of moving into a facility, a person receives structured treatment while continuing to live at home. That means care can happen alongside ordinary responsibilities, with a schedule built around the level of support needed.
Practical rule: The right program shouldn't force a false choice between getting help and handling life. It should match the level of care to the level of risk.
For a working professional in Euless, outpatient rehab may mean attending therapy and group sessions several days a week, then going home at night. For a college student in Dallas, it may mean receiving treatment while staying connected to classes and family support. For a parent, it may mean finally getting clinical help without disappearing from the household.
Recovery doesn't happen in a vacuum. People still have stress, routines, relationships, and triggers, making real-time application of coping skills essential. Outpatient treatment gives them a place to work on those issues as they arise. They can talk through a difficult conversation, a commute trigger, a family conflict, or a weekend craving, then practice new coping skills in daily life instead of waiting until treatment ends.
That's one reason outpatient care has become the foundation of addiction treatment in the United States. It is widely available and designed to meet people where they are, not where they wish their life circumstances were.
Understanding the Levels of Outpatient Care
Not all outpatient rehab looks the same. That's where many readers get stuck. They hear “outpatient” and assume it means one weekly therapy session. In reality, outpatient care includes several levels, each with a different amount of structure and support.
A useful way to think about it is physical rehabilitation after an injury. Some people need daily intensive support at first. Others need a moderate schedule while they rebuild strength. Others are ready for periodic follow-up. Addiction treatment often works the same way.
Why there are different levels
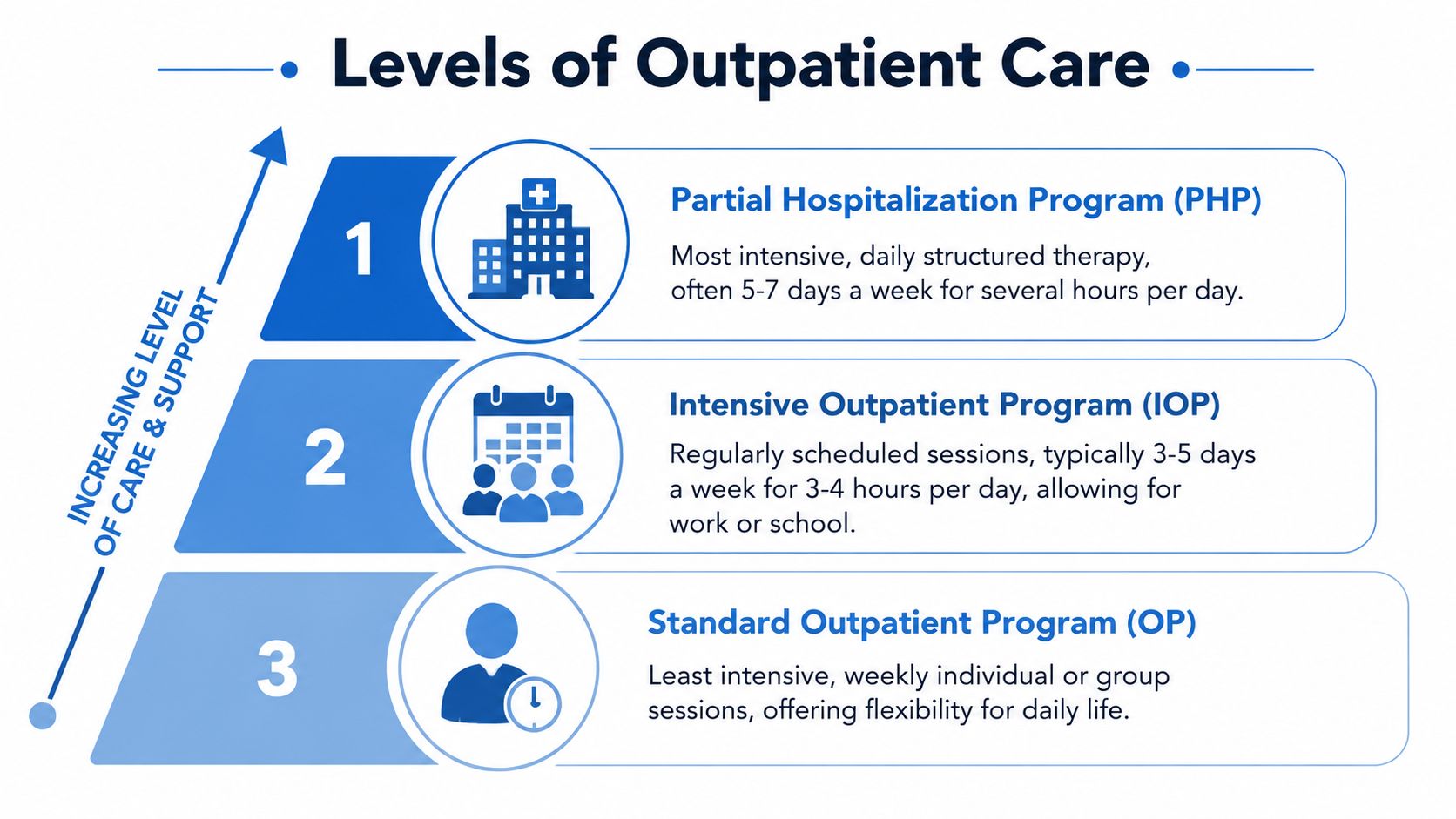
Partial Hospitalization Program or PHP is the most intensive outpatient level. A person attends treatment for much of the day, several days each week, but still returns home in the evening. PHP often fits people who need strong structure, close monitoring, and a substantial amount of therapy without full residential care.
Intensive Outpatient Program or IOP steps down from that. It still provides a meaningful amount of treatment, but with more room for work, school, or family responsibilities. According to research on intensive outpatient programs, IOPs typically provide 9 to 15 hours of therapy per week, and longer treatment duration is associated with 20 to 30% better social functioning. That same research notes that IOP outcomes can be comparable to inpatient programs for reductions in substance use.
Standard outpatient care is the least intensive level. It may involve weekly individual counseling, group therapy, medication management, or ongoing recovery support. This level often works well as continuing care after PHP or IOP, or for someone whose needs are stable and manageable with less frequent contact.
A person doesn't have to guess where they belong. Clinical assessment is what determines whether someone should start at PHP, begin with IOP, or move into standard outpatient. For readers trying to understand the middle tier, this guide to what IOP therapy involves can help make the structure more concrete.
A simple way to compare options
| Level of Care | Time Commitment | Living Situation | Best For |
|---|---|---|---|
| PHP | Most of the day, several days each week | Lives at home | People who need high structure and close support |
| IOP | Multiple sessions each week | Lives at home | People who need strong treatment but must keep daily responsibilities |
| Standard Outpatient | Fewer scheduled sessions | Lives at home | People stepping down in care or needing ongoing support |
| Inpatient Rehab | Full-time treatment | Lives on site | People who need 24/7 supervision and a fully controlled setting |
The level of care is not a grade on how “bad” things are. It's a matching process. The question is how much support helps a person stay safe and engaged in recovery right now.
One of the strengths of outpatient treatment is that it can change as recovery changes. A person might begin in PHP, build stability, move into IOP, and then continue in standard outpatient care. That step-down model gives recovery structure without making the transition abrupt.
What a Week in Outpatient Rehab Looks Like
The phrase “outpatient rehab” can still sound vague until it becomes concrete. Prospective participants often want to know what takes place during the week, who they'll meet with, and whether it will feel cold or impersonal.
A typical outpatient week blends several types of care. Instead of doing the same thing every day, treatment usually combines therapy, skill building, peer support, and case-specific services such as medication management or dual diagnosis care.
What happens during sessions
One part of the week is often individual therapy. That's where a person can speak privately about relapse triggers, trauma, shame, family conflict, work stress, or fear about the future. This is usually where treatment becomes personal instead of generic.
Another part is group therapy. Some people dread this before starting, but group sessions often become the place where isolation begins to break. Hearing other people describe the same cravings, lies, guilt, or anxiety can reduce the feeling of being uniquely broken.
A week may also include:
- Psychoeducation: learning how substance use affects the brain, body, mood, and decision-making.
- Relapse prevention planning: identifying warning signs, high-risk situations, and practical responses.
- Family involvement: when appropriate, loved ones may join parts of treatment to improve communication and rebuild trust.
- Mental health support: if depression, anxiety, trauma, or another condition is present, care should address both issues together rather than treating addiction in isolation.
A person in IOP, for example, might attend several sessions across the week, with a mix of group work and one-on-one appointments. Someone in standard outpatient may have fewer visits but continue practicing coping skills between sessions in daily life.
When MAT is part of the plan
For opioid use disorder, medication-assisted treatment or MAT can be a critical part of outpatient rehab. MAT may include medications such as Suboxone as part of a broader treatment plan that also includes counseling and monitoring. According to outpatient MAT data and treatment statistics, outpatient MAT for opioid detox has a 41% successful completion rate, and long-term research shows MAT helps prevent overdose deaths.
That matters because treatment isn't just about willpower. For some people, reducing cravings and withdrawal symptoms can make it possible to stay engaged long enough for therapy and behavior change to take hold.
Recovery often becomes more manageable when treatment lowers the daily noise of cravings, panic, and withdrawal. Then a person can actually focus on the work of getting better.
A good outpatient week should feel structured, but not chaotic. It should challenge the person, while still allowing enough room to return home, go to work, care for children, attend school, and start applying what they're learning in real life.
Outpatient Versus Inpatient The Right Choice for You
This decision is rarely about which option sounds more appealing. It's about which environment gives a person the safest and most realistic chance to stabilize.
Some people do very well in outpatient care. Others need the protection and intensity of inpatient treatment first. There's no shame in either path.
When outpatient makes sense
Outpatient rehab may be a strong fit when a person has some stability at home, can attend scheduled care reliably, and needs treatment that works around life responsibilities. It can also be a practical option for people stepping down from a higher level of care.
Some signs outpatient may fit include:
- A workable home environment: home isn't perfect, but it's safe enough to support recovery.
- Daily responsibilities that can't be abandoned: work, school, parenting, or caregiving still need attention.
- Motivation for treatment: the person is willing to participate, show up, and follow a treatment plan.
- Need for ongoing reintegration: the person benefits from practicing coping skills in normal life right away.
When a higher level of care may be safer
Inpatient care may be more appropriate when substance use is severe, the living environment is unstable, medical needs are complex, or relapse risk is high without full-time support. A person who cannot stay safe outside a structured setting may need inpatient stabilization before outpatient can work.
One issue many families don't hear enough about is the transition itself. According to guidance on inpatient and outpatient rehab transitions, people often struggle when stepping down from 24/7 inpatient support, and continuity with the same team and plan can play an important role in relapse prevention.
That means the handoff matters. If someone leaves a highly structured setting and enters outpatient care without a clear plan, medication continuity, and therapeutic connection, the risk can rise during that unstable period. For readers comparing settings, this overview of the difference between inpatient and outpatient treatment can help frame the decision in practical terms.
The safest plan is often not one level of care forever. It's a continuum that adjusts as the person becomes more stable.
The right question isn't “Which option is easier?” It's “Which option matches the current level of medical, emotional, and environmental risk?”
How to Choose a Quality Program in Dallas-Fort Worth
Once a person understands what outpatient rehab is, the next challenge is choosing wisely. Programs can sound similar on the phone, but the actual quality of care can be very different.
The strongest programs don't just offer sessions on a calendar. They assess carefully, personalize treatment, track progress, and adjust when something isn't working.
Questions worth asking before admission
A family looking in Euless or the larger DFW area should ask direct questions:
- Is treatment individualized: Does the program create a real plan based on substance use history, mental health needs, relapse risk, and daily responsibilities?
- Are evidence-based therapies used: A quality program should be able to explain the therapeutic methods it relies on in plain language.
- How are care transitions handled: If someone needs to move from PHP to IOP, or from inpatient into outpatient, is that change organized or improvised?
- What does dual diagnosis care look like: If anxiety, depression, trauma, or another condition is present, both issues should be treated together.
- How does insurance verification work: The admissions process should explain benefits, coverage questions, and financial expectations clearly.
These questions help separate generic scheduling from actual clinical planning.
Why personalization matters
Treatment works better when it fits the person in front of the clinician. According to data on personalized addiction treatment and outcomes tracking, data-driven personalization can increase success rates by 10 to 20%, and facilities using validated tools report 25% superior outcomes. That same source notes that individualized MAT interventions can cut cravings by 50 to 70%.
Those numbers point to a practical reality. A person with opioid use and strong cravings may need a different plan than someone with alcohol use and untreated trauma. A parent with a rigid work schedule may need a different attendance structure than a college student. A person stepping down from inpatient care needs a different bridge than someone starting treatment for the first time.
A local example is Maverick Behavioral Health, which provides PHP, IOP, and standard outpatient care in the Euless area with dual diagnosis treatment, MAT support, and individualized planning based on clinical needs.
The best admissions conversations feel calm, not pressured. Staff should answer plainly, explain levels of care, and help the person understand what the first week will look like.
Begin Your Recovery in Euless with Maverick Behavioral Health
You may be sitting at your kitchen table after a hard week, knowing something needs to change, but unsure how treatment would fit into real life. The first question is often not "What is rehab?" It is "How do I start without dropping everything, and what happens if my needs change after I begin?"
For adults in Euless and across Dallas-Fort Worth, local care matters because recovery rarely stays at one intensity from day one to discharge. Early on, you may need more structure. A few weeks later, you may be ready for fewer hours while still keeping close clinical support. That step-down process matters because gaps between levels of care can leave people feeling unsteady right when they are trying to build momentum.
What local outpatient care should include
A strong outpatient program should make it possible to move from one level of care to another without confusion or delays. Recovery often works like learning to walk after an injury. At first, you may need more support and closer supervision. As you regain stability, the support should adjust, not disappear.
That is why it helps when one provider can offer PHP, IOP, and standard outpatient care in the same setting. If your schedule, symptoms, cravings, or home stressors change, your treatment plan can change with them. You do not have to start over with a new team each time your level of care shifts.
Good outpatient treatment should also address the issues that often show up alongside substance use. That can include therapy for anxiety, depression, or trauma, counseling focused on daily triggers and relapse patterns, and medication support when it fits your clinical needs.
For many people, continuity is what makes treatment feel manageable. You learn the routines. You know the staff. Your care plan keeps building instead of restarting.
A simple next step
If you are trying to sort this out while managing work, family, or fear about what comes next, a short admissions call can help turn uncertainty into a plan. The goal is not to pressure you. The goal is to help you understand what level of care may fit now, how insurance may apply, and how treatment could continue if you later step down from PHP to IOP or from IOP to outpatient support.
You can review outpatient rehab options in Euless and Tarrant County to get a clearer picture of what care may look like close to home. If you are ready to talk it through, call (888) 385-2051 and ask for a confidential consultation.
Frequently Asked Questions About Outpatient Rehab
Can someone keep a job while in outpatient rehab
Often, yes. That's one of the main reasons people choose outpatient treatment. The schedule is built so a person can receive care and still live at home. The exact fit depends on the level of care, work hours, transportation, and clinical needs.
How long does outpatient rehab last
There isn't one fixed timeline for everyone. Length depends on the level of care, the substance involved, mental health needs, progress in treatment, and whether the person is stepping down from a more intensive program. In many cases, treatment lasts longer when a person needs more support early and then tapers gradually instead of ending abruptly.
How do insurance and first calls usually work
Most first calls focus on basic screening, scheduling, and insurance verification. The admissions team typically asks about substance use, safety concerns, mental health symptoms, prior treatment, and availability. From there, they can explain possible next steps and what level of care may fit.
For someone who feels overwhelmed, the first goal doesn't need to be solving everything at once. It only needs to be starting the conversation. A confidential call can turn a vague fear into a clear plan.
If outpatient treatment may be the right fit, Maverick Behavioral Health offers confidential guidance for adults in Euless and the Dallas-Fort Worth area. A quick call to (888) 385-2051 can help clarify options, review insurance, and identify the next appropriate step in care.