A lot of people land on this question in a moment of uncertainty. A student in Dallas takes Adderall to stay focused for a late study session, then goes out for drinks. A young professional in Euless uses a prescription stimulant during a long workday, then joins friends at a happy hour and assumes staying alert means staying safe.
That assumption is where the danger starts. Mixing alcohol and adderall can feel less risky than it really is because the body sends mixed signals. Someone may look awake, sound more put together, and feel “fine,” while their alcohol level and physical stress are moving in the wrong direction.
The concern isn’t rare or limited to one type of person. According to SAMHSA data summarized by American Addiction Centers, 3.7% of full-time college students engaged in nonmedical prescription drug use, like Adderall, in the past month, and that misuse is strongly linked with alcohol consumption. For families, partners, and friends, that helps explain why this question comes up so often. It also shows why clear, non-judgmental education matters.
Table of Contents
- The Hidden Dangers of a Common Combination
- How Your Body Processes Alcohol and Adderall Together
- Short and Long-Term Health Consequences
- Recognizing the Warning Signs of a Problem
- What to Do in an Emergency Situation
- How to Find Lasting Recovery in Dallas-Fort Worth
- Take the First Step Toward a Safer Future
The Hidden Dangers of a Common Combination
A common pattern looks harmless on the surface. Someone takes Adderall in the afternoon to study, finish a deadline, or push through exhaustion. Hours later, drinks enter the picture, and the person believes the stimulant will keep them sharp enough to handle the alcohol.
That belief can be persuasive because the person may still be talking quickly, moving normally, and insisting they aren’t that drunk. Friends may believe it too. From the outside, the situation can look controlled even when it isn’t.
What makes this combination different from many other risky choices is that it doesn’t just add one substance to another. It changes the way intoxication is experienced. The body may be under significant strain while the mind feels unusually confident.
A false sense of sobriety is not real safety. It’s one of the most dangerous features of mixing alcohol and adderall.
This is one reason families often miss the problem until something more serious happens. They may notice staying out later, drinking more than expected, or acting impulsively, but they may not realize the stimulant is helping hide alcohol’s usual warning signs.
In the Dallas-Fort Worth area, this can affect more than college students. It can involve people with legitimate prescriptions, shift workers trying to stay functional, or adults who think a few drinks after taking medication won’t matter. The context changes, but the risk remains.
Why people underestimate it
Several misunderstandings show up again and again:
- “The stimulant cancels out the alcohol.” It doesn’t. The two drugs send conflicting signals through the body.
- “If someone is awake and talking, they must be okay.” Alertness doesn’t equal safety.
- “It only counts as misuse if the Adderall wasn’t prescribed.” Even prescribed use paired with drinking can create dangerous effects.
- “They would know if they were in trouble.” That’s exactly the problem. The mix can make a person feel less impaired than they are.
People usually aren’t trying to create a medical crisis. Many are trying to study longer, socialize harder, stay energized, or avoid feeling as drunk. Those motives can seem ordinary. The outcome can still become life-threatening.
How Your Body Processes Alcohol and Adderall Together
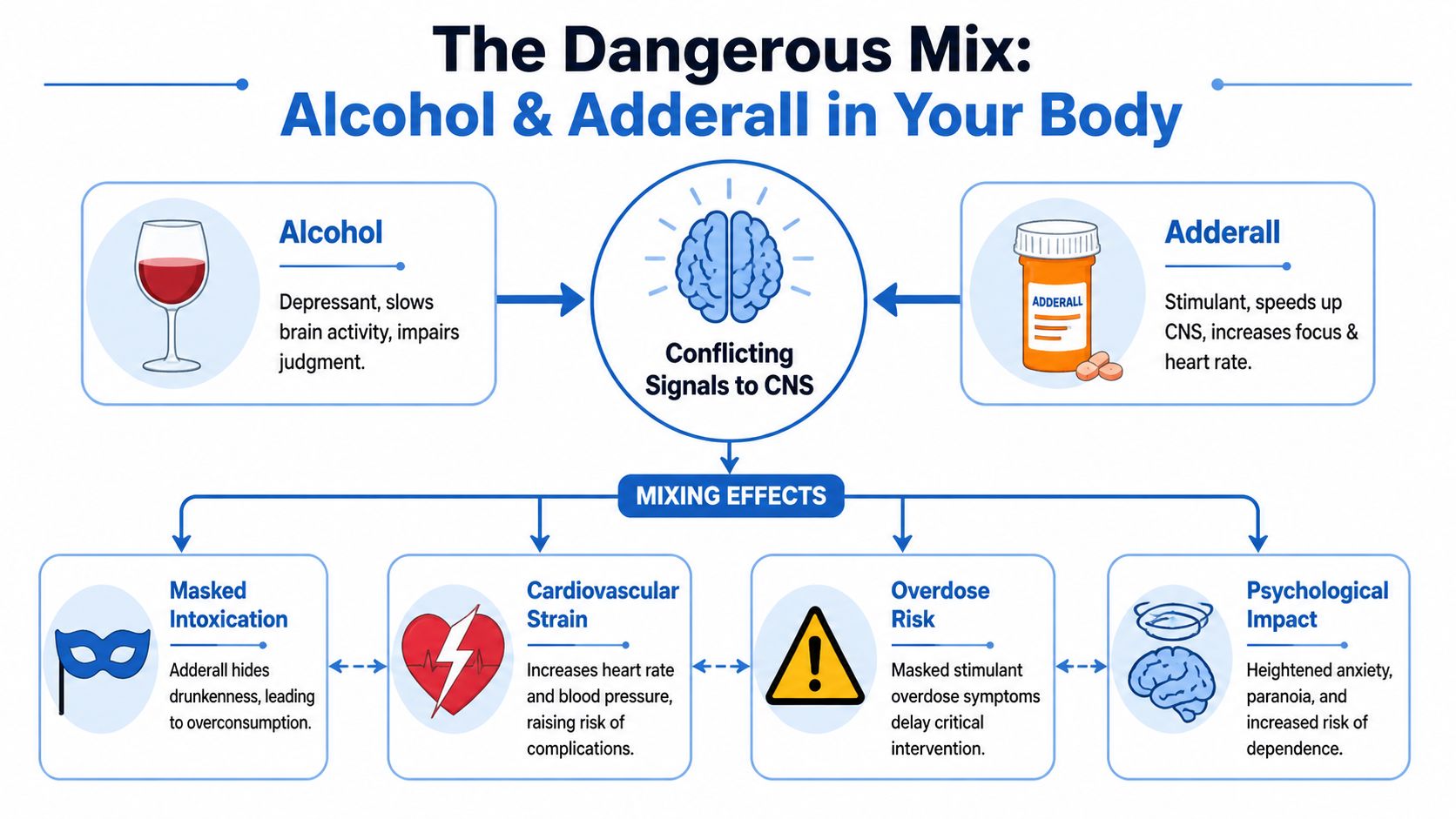
Alcohol and Adderall pull the body in opposite directions. Alcohol is a depressant. Adderall is a central nervous system stimulant. When both are active at the same time, the body doesn’t settle into a safe middle ground.
A simple comparison helps. It’s like driving with one foot on the gas and one foot on the brake. The car doesn’t become stable. It becomes harder to control, and the strain on the system goes up.
Why opposite effects don’t balance out
Adderall tends to increase alertness, heart rate, and blood pressure. Alcohol slows brain activity, lowers inhibitions, and impairs judgment and coordination. Those effects don’t erase each other. They overlap in a way that confuses the person taking them.
The result is often a person who feels more capable than they are. They may decide to keep drinking because they don’t feel sleepy, clumsy, or obviously intoxicated. They may think they can drive, keep up socially, or safely handle “just one more.”
That’s why the combination can fool both the person using it and the people around them. The usual signs many people rely on to judge drunkenness may be less visible.
How false sobriety happens
When mixed, Adderall’s stimulant properties suppress the usual warning signs of alcohol intoxication, such as drowsiness and impaired motor control. That can lead a person to consume dangerous amounts of alcohol without realizing how intoxicated they really are, as explained in Alcohol Help’s discussion of Adderall and alcohol.
This is the core danger. The brain and body normally provide feedback that says, slow down, sit down, stop drinking, something’s wrong. With this combination, those signals can be dulled or hidden.
A reader may wonder whether this is just “high tolerance.” It isn’t necessarily tolerance. It can be a masking effect, where the stimulant changes the person’s perception of how impaired they are.
Someone who says, “I don’t even feel drunk,” may be describing the danger, not disproving it.
That false sobriety can lead to several risky decisions in a short span of time. A person may keep drinking, mix in another substance, get behind the wheel, become sexually impulsive, or ignore chest discomfort and agitation because they still feel functional. By the time the body’s distress becomes obvious, the situation may already be an emergency.
Short and Long-Term Health Consequences
The health effects of this combination often show up in two ways. Some risks appear quickly, within the same night. Others develop with repeated use and can continue affecting a person long after the party, exam week, or stressful period has ended.
Short-term risks that can turn serious fast
The immediate danger often starts with overdrinking. Because the person doesn’t feel as sedated as expected, they may continue consuming alcohol past the point where they would normally stop. That raises the risk of alcohol poisoning, blackout behavior, vomiting, collapse, injury, and overdose.
Poor judgment is another major concern. Someone may feel energized and socially confident while experiencing considerable impairment. That can lead to unsafe driving, falls, fights, risky sexual behavior, or impulsive decisions that would have seemed obviously dangerous if alcohol’s effects were more visible.
Short-term warning signs can include:
- Rapid heartbeat: A person may complain that their heart is racing or pounding.
- Agitation or restlessness: They may look keyed up rather than drunk.
- Confusion: Speech may still seem animated, but judgment can be badly impaired.
- Sudden physical decline: Vomiting, collapse, slowed breathing, or unresponsiveness can follow after a period of seeming “fine.”
Important: Staying awake doesn’t protect someone from alcohol poisoning.
Long-term damage that builds with repeated use
The mix of Adderall and alcohol creates significant cardiovascular stress. Acute effects include increased heart rate, high blood pressure, and heart palpitations. Repeated misuse leads to sustained strain on the heart and can cause long-term central nervous system damage, compromising cognitive function and increasing seizure risk, according to GoodRx’s review of Adderall and alcohol effects.
That means the risk isn’t limited to one bad night. A repeated pattern can affect concentration, memory, mood stability, and physical health over time. Some people begin using one substance to manage the aftereffects of the other. They may use Adderall to push through exhaustion or brain fog, then use alcohol to come down, sleep, or blunt anxiety. That cycle can become hard to interrupt without treatment.
For people with ADHD, anxiety, depression, or another co-occurring condition, the picture may become even more complicated. The person may believe they are self-managing stress or performance demands when they are instead deepening both the mental health problem and the substance use problem.
Risks of mixing alcohol and Adderall
| Risk Type | Examples |
|---|---|
| Immediate intoxication risk | Drinking more than intended, blackouts, alcohol poisoning, collapse |
| Behavioral risk | Unsafe driving, impulsive choices, aggression, unsafe sex |
| Cardiovascular risk | Elevated heart rate, high blood pressure, heart palpitations, chest pain |
| Neurological risk | Impaired judgment, cognitive problems, increased seizure risk |
| Addiction-related risk | Escalating use, using one substance to manage the other, difficulty stopping |
A person doesn’t need to “look addicted” for this pattern to become dangerous. Repeated close calls, using the combination to function, or needing it to get through social or academic pressure are all signs that the problem may be growing.
Recognizing the Warning Signs of a Problem
Many people don’t recognize the issue at first because the pattern can hide in plain sight. A person may still go to work, attend class, answer texts, and show up socially. What changes first is often the pattern around the substances, not the person’s whole life all at once.
Sometimes family members only realize something is wrong after a string of small incidents. Missed responsibilities. Mood changes. Nights that end in conflict or confusion. A person who insists they are in control may still be showing a clear pattern that needs attention.
Readers who want a broader look at substance use red flags can review these signs that someone may need rehab.
Physical warning signs
Some signs show up in the body first.
- Heart-related symptoms: racing heartbeat, pounding chest, palpitations, or unexplained chest discomfort
- Sleep disruption: trouble falling asleep, staying asleep, or “crashing” after periods of stimulation
- Changes in energy: alternating between overactivated and drained
- Visible instability: shakiness, sweating, dehydration, nausea, or repeated hangovers that seem unusually severe
Behavioral changes
Other signs show up in choices and routines.
- Drinking more than planned: the person repeatedly says they only meant to have a little
- Using Adderall around drinking on purpose: before parties, nights out, or situations where they want to stay awake longer
- Hiding use: minimizing, denying, or becoming defensive when asked about pills or alcohol
- Neglecting responsibilities: slipping performance, missed deadlines, strained relationships, or unsafe decisions
Psychological signs
This combination can also affect mood and thinking in ways that loved ones notice before the person does.
- Anxiety: more tension, panic, or fear after nights of drinking and stimulant use
- Irritability: sudden anger, impatience, or conflict
- Paranoia or suspiciousness: especially after heavy use or poor sleep
- Depression or emotional crash: guilt, hopelessness, or feeling flat after the substances wear off
If a person needs Adderall to keep drinking or alcohol to come down from Adderall, that pattern usually isn’t casual anymore.
A warning sign doesn’t have to be dramatic to matter. Repetition is often what reveals the problem. The same risky choice, the same excuse, the same fallout. When that loop is visible, it’s time to stop treating it like a phase.
What to Do in an Emergency Situation
When someone may be in crisis after mixing alcohol and adderall, speed matters. It’s safer to treat the situation as an emergency than to wait and hope they “sleep it off.”
When to call 911
Call 911 right away if the person is showing any of these signs:
- Unresponsiveness: they can’t be woken up or won’t stay awake
- Breathing problems: breathing is slow, irregular, shallow, or seems to stop
- Seizure activity: any seizure or sudden convulsions
- Blue, pale, or cold skin: especially around the lips or fingertips
- Repeated vomiting: especially if the person is drowsy, confused, or hard to rouse
- Collapse or extreme confusion: they can’t stand, speak clearly, or track what’s happening
What to do while help is on the way
Keep the steps simple and focused.
- Stay with the person. Don’t leave them alone.
- Turn them on their side if they are vomiting or very drowsy. This can reduce choking risk.
- Tell emergency responders what was taken if known. Medication name, alcohol use, and timing can help.
- Keep the environment calm. Reduce noise and stimulation.
- Watch breathing and responsiveness until help arrives.
What not to do matters too:
- Don’t assume sleep will fix it.
- Don’t give more alcohol, more medication, or other substances.
- Don’t force vomiting.
- Don’t rely on coffee, food, or a shower to reverse intoxication.
- Don’t let the person drive or walk away.
A person can be in medical danger even if they’re still talking.
If there’s any doubt, emergency evaluation is the right call. It’s better to have professionals assess the person than to miss the point where the body starts shutting down.
How to Find Lasting Recovery in Dallas-Fort Worth
For many adults in Euless, Dallas, and the surrounding metroplex, the biggest barrier to treatment isn’t denial alone. It’s logistics. People worry about work, classes, family obligations, privacy, and whether the problem is “serious enough” to justify help.
Those concerns are common, but they don’t have to delay care. Treatment for mixing alcohol and adderall can be practical, flexible, and designed to fit the life a person is already living.
Why outpatient care fits many adults in DFW
Outpatient treatment can make sense for people who need meaningful support without stepping away from everyday responsibilities completely. Someone may need structured therapy, relapse prevention, accountability, and psychiatric support while still maintaining school, work, or home responsibilities.
In the Dallas-Fort Worth area, that often means looking for care options such as:
- Partial Hospitalization Program care: a higher level of support during the day without overnight residence
- Intensive Outpatient Program care: a structured option for people who need more than weekly therapy
- Standard outpatient services: ongoing counseling and support for continued recovery work
This is especially important when alcohol and stimulant use overlap with ADHD, anxiety, depression, trauma, or another mental health concern. In those cases, treating only the substance use problem may leave the person vulnerable to relapse because the underlying drivers remain active.
What effective care often includes
A strong treatment plan usually addresses both safety and the reasons the pattern developed.
Some people need help sorting out whether they are misusing a prescription, self-medicating stress, or using substances to keep up with school or work pressure. Others need dual diagnosis support because concentration problems, mood symptoms, and substance use are intertwined.
Helpful treatment elements may include:
- Clinical assessment: identifying substance use patterns, mental health symptoms, and medical risk
- Dual diagnosis care: treating co-occurring mental health conditions alongside substance use
- Medication support when appropriate: especially when withdrawal, cravings, or psychiatric symptoms need careful management
- Skills-based therapy: learning how to manage stress, social pressure, sleep disruption, and urges without cycling between substances
- Aftercare planning: building a recovery routine that fits daily life in the community
Readers looking for local guidance on treatment for prescription medication misuse can review prescription medication rehab options in Dallas and Dallas County.
Recovery doesn’t always begin with a dramatic rock-bottom moment. It often begins when a person finally admits that the “I’m fine” feeling can’t be trusted anymore.
Take the First Step Toward a Safer Future
The central risk of mixing alcohol and adderall is deceptive. The danger often doesn’t feel dangerous at first. A person may seem alert, confident, and functional while their judgment, alcohol intake, and physical stress are moving into unsafe territory.
That’s why waiting for the problem to become obvious can be costly. The false sense of sobriety can delay help, minimize warning signs, and keep a harmful pattern going longer than the person or family expected. What looks manageable on the surface may already be affecting safety, health, school, work, or relationships.
There is another path. With the right support, people can stop the cycle, understand what has been driving the behavior, and build a recovery plan that fits real life. That may include outpatient care, dual diagnosis treatment, medication support, therapy, or a combination of services based on individual needs.
For anyone in Euless, Dallas, or the surrounding DFW area who is unsure whether it’s time to act, a confidential admissions conversation can provide clarity. Starting that process doesn’t commit anyone to treatment on the spot. It opens the door to honest guidance and next steps.
A helpful place to start is the admissions page for treatment options and support. For immediate guidance, call (888) 385-2051.
Maverick Behavioral Health provides compassionate outpatient substance use and mental health treatment for adults in Euless, Dallas, and the greater Dallas-Fort Worth area. Anyone concerned about mixing alcohol and adderall can call (888) 385-2051 for a confidential conversation about treatment options, dual diagnosis support, and the next safe step forward.