A family in Plano usually doesn’t start searching for treatment on a good day. The search often begins late at night, after another broken promise, another frightening call, another sign that alcohol or drugs have taken over more of life than anyone wanted to admit. Then the browser fills with options. Detox. PHP. IOP. Dual diagnosis. Insurance accepted. Luxury. Evidence-based. It all starts to blur.
That’s where many individuals get stuck. They aren’t just looking for rehab centers in Plano Texas. They’re trying to figure out which option fits real life, protects a career, supports mental health, and gives someone a genuine shot at staying sober after treatment ends.
The right way to approach this decision is practical, not flashy. The Dallas-Fort Worth area gives families a lot of choices. What matters is knowing how to sort those choices fast, and how to recognize an outpatient program that can support long-term recovery for a working adult, student, parent, or anyone managing both substance use and mental health symptoms.
Table of Contents
- Finding Hope and Help for Addiction in Plano Texas
- The Advantage of Outpatient Rehab in the Dallas-Fort Worth Area
- Understanding Your Treatment Options PHP versus IOP
- Four Pillars of High-Quality Addiction Treatment
- Critical Questions to Ask Before You Enroll
- Your Path to Recovery Starts Here How to Get Started
- Frequently Asked Questions About Rehab in Plano TX
- Can someone keep a job while attending an IOP program
- Is outpatient treatment enough for serious addiction
- What if mental health is part of the problem
- Does family involvement matter
- What types of insurance are usually accepted
- How long does treatment last
- What should a family do today if they’re overwhelmed
Finding Hope and Help for Addiction in Plano Texas
It usually starts with a call after a hard night. A spouse says things are getting worse. A parent says their son still goes to class but is not himself. A professional says work is holding together, barely. In Plano, that pattern is common. People can look functional long after substance use has become dangerous.
That is why families need a decision process, not another list of rehab centers. Plano is a large, fast-moving city in Collin County, with a population estimated by the U.S. Census Bureau. The pressure to keep performing here is real. So is the tendency to hide a problem until it disrupts health, work, marriage, or parenting.
The local need is real
North Texas families are not overreacting when they treat substance use as urgent. Texas recorded more than 5,000 drug overdose deaths in 2022, according to the Texas overdose data summarized by state and local reporting. That is the right backdrop for this decision. Waiting for a dramatic collapse is a mistake.
Use a simple standard. If alcohol or drug use is affecting safety, sleep, mood, work, school, money, or trust at home, get an assessment now.
For many families in Plano, Frisco, Allen, McKinney, and North Dallas, the right next step is not detox or inpatient by default. It is a structured outpatient program that can treat addiction and mental health at the same time while life keeps moving. If that sounds like your situation, review what a strong outpatient rehab program in Dallas County should include before you enroll anywhere.
Hope starts with clarity
Hope is not wishful thinking. Hope is knowing what to ask and what to rule out.
Start with these questions:
- Can the person stay safe outside of treatment hours? If safety is uncertain, do not force a low-intensity option.
- Is there depression, anxiety, trauma, burnout, or another mental health issue in the picture? Working professionals and high-functioning adults often need dual-diagnosis care, not addiction treatment alone.
- Does the person need to keep working, parenting, or attending school? In the Plano and Dallas area, practical fit matters. A program that disrupts life so much that the person quits is the wrong program.
- Has treatment or sobriety support failed before because the step-down was too fast or too generic? That usually points to poor program design, not a lack of motivation.
Families searching for rehab centers in Plano Texas need clear guidance. Choose a program that matches the person’s risk level, treats co-occurring disorders directly, and works for real life in DFW. That is how you stop guessing and start getting traction.
The Advantage of Outpatient Rehab in the Dallas-Fort Worth Area
It is 6:30 a.m. in Plano. A parent is packing lunches, checking work emails, and wondering how treatment could possibly fit into an already overextended week. That is the reality for many families in DFW. They need real addiction treatment, but they also need a plan that can survive Monday morning.
For many adults in Plano, Dallas, Euless, and nearby communities, outpatient rehab is the right starting point. It allows treatment to happen in real life, where stress, triggers, work pressure, family conflict, and mental health symptoms show up. That matters even more for working professionals and for people dealing with both substance use and depression, anxiety, trauma, or burnout.
Why outpatient fits the DFW reality
The Dallas-Fort Worth area gives families more than one treatment path. SAMHSA’s treatment locator shows a broad mix of outpatient providers across the region, which is one reason many families start by comparing schedule, clinical depth, and mental health support instead of assuming residential care is the only serious option: find outpatient and other treatment services in the Dallas-Fort Worth area.
That practical fit is the primary advantage.
A good outpatient program lets someone stay connected to work, school, parenting, or home responsibilities while still receiving structured care several days each week. For a high-functioning adult, that often produces better honesty and better clinical insight. The person is not isolated from daily pressure. They are learning how to respond to it without drinking, using, shutting down, or spiraling.
Outpatient care also makes it easier to spot whether the problem is only substance use, or substance use plus a co-occurring disorder that has been driving the cycle for years.
What families should value most
Do not choose outpatient care because it looks convenient. Choose it when the person can remain safe outside program hours and needs a treatment model that can hold up under real-world pressure.
The best outpatient programs tend to offer four practical advantages:
- Treatment that works around employment: Professionals often need day or evening options, clear attendance expectations, and privacy.
- Direct family involvement: Partners and relatives can be brought into the process while patterns are still happening at home.
- Immediate use of coping skills: Clients practice communication, craving management, boundary-setting, and relapse prevention in the same environments that have been causing problems.
- Better long-term fit for dual diagnosis care: Ongoing therapy and psychiatric coordination are often easier to maintain in outpatient treatment than in short, disconnected episodes of care.
If you are comparing options, this overview of an outpatient rehab program in Dallas County gives a useful picture of what structured outpatient care should include.
Outpatient care requires more than attendance
Families often underestimate this level of care. They should not.
Strong outpatient treatment is disciplined, clinical, and accountable. It should include individual therapy, group therapy, relapse prevention work, treatment planning, and mental health support when needed. For adults with co-occurring disorders, outpatient care can be especially effective because clinicians can see how symptoms show up between sessions, not just inside a controlled setting.
That makes treatment more honest. It also makes it more useful.
Who tends to benefit most
Outpatient rehab deserves serious consideration for people who need meaningful treatment without stepping away from life completely:
- Working professionals who need structure without abandoning their job
- Parents and caregivers who need care that fits family responsibilities
- College students or graduate students who need support without losing academic momentum
- Adults stepping down from residential treatment who still need frequent clinical contact
- People with co-occurring mental health symptoms who need addiction and psychiatric care addressed together
The right program does not force everyone into the same schedule or intensity. It matches the person’s stability, responsibilities, and symptom pattern. That is why outpatient rehab remains one of the strongest options for families searching for rehab centers in Plano Texas.
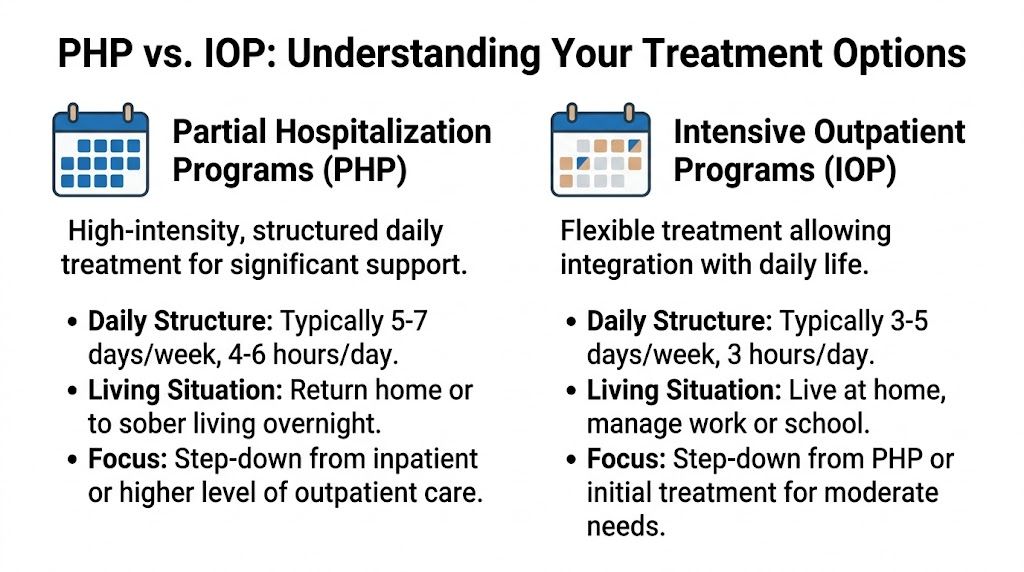
Understanding Your Treatment Options PHP versus IOP
Most families hit the same wall after deciding on outpatient care. They understand they want treatment, but they don’t know whether PHP or IOP makes sense. That decision matters.
Pick too little support, and the person may stay overwhelmed. Pick too much structure for the wrong situation, and treatment can become hard to sustain. The answer isn’t based on pride or convenience. It should be based on current stability, symptom severity, and how much support the person needs to stay engaged.
Comparing PHP and IOP Levels of Care
| Feature | Partial Hospitalization Program (PHP) | Intensive Outpatient Program (IOP) |
|---|---|---|
| Structure | High structure during the day | Moderate structure on scheduled treatment days |
| Typical schedule | Often runs most weekdays for several hours each day | Often runs fewer days per week for shorter blocks |
| Best fit | People who need strong support but don’t require 24-hour residential care | People who need consistent treatment while managing work, school, or family |
| Living situation | Client returns home or to sober living after programming | Client lives at home or in supportive housing |
| Clinical intensity | Higher | Moderate but still substantial |
| Common use | Step-down from inpatient care or a starting point for someone needing close monitoring | Step-down from PHP or a starting point for someone with more stability |
| Goal | Stabilization and daily therapeutic engagement | Ongoing recovery work with greater real-world integration |
A practical explanation of what is IOP therapy can help clarify how this level of care fits into recovery planning.
Who usually fits PHP better
PHP is the better option when a person needs a lot of structure but doesn’t need overnight residential supervision.
That often includes people who are newly sober, people whose cravings are still intense, and people whose mental health symptoms are interfering with daily functioning. It can also fit someone leaving inpatient treatment who still feels shaky.
PHP usually makes more sense when the person is dealing with issues like:
- Unstable early recovery: They’ve stopped using, but they’re not steady yet.
- High relapse risk: Triggers are everywhere and coping skills are weak.
- Significant co-occurring symptoms: Depression, anxiety, trauma responses, or mood instability still need close attention.
- Recent treatment transition: They’re leaving detox or residential care and need a strong landing place.
A family should take PHP seriously if home life is supportive enough for evenings, but the person still needs a treatment-heavy week.
Who usually fits IOP better
IOP works best when the person has enough stability to manage treatment alongside daily responsibilities. That doesn’t mean the addiction is mild. It means the person can function safely between sessions with the right support.
IOP often fits adults who need serious help but also need to keep some normal routines intact.
Examples include:
- A professional who can’t leave work entirely but clearly needs more than weekly therapy.
- A student whose substance use is affecting performance but who still has enough daily stability to stay engaged.
- A parent with dependable home support who needs regular treatment without full daytime programming.
- Someone stepping down from PHP who’s ready for more independence without losing accountability.
A good admissions team won’t sell a level of care. They’ll match one.
What families should use to decide
The simplest way to choose between PHP and IOP is to focus on function, not labels.
Ask these questions:
- Can the person stay sober and safe outside of sessions right now?
- Are mental health symptoms disrupting sleep, work, relationships, or judgment?
- Has a lower level of care already failed?
- Would the person benefit from treatment most days of the week, or can they manage with fewer treatment days and strong follow-through?
If the answer to those questions points to instability, PHP is usually the stronger starting point. If the person has more traction, more support, and more day-to-day reliability, IOP may be the right fit.
Families looking at rehab centers in Plano Texas should not treat PHP and IOP like interchangeable menu items. They solve different problems. The best outcome often comes from starting with the right intensity, then stepping down as stability improves.
Four Pillars of High-Quality Addiction Treatment
A polished website proves almost nothing. The right outpatient program proves itself in the clinical work, in how it responds when cravings surge, mood symptoms flare, or a working professional starts slipping at home and at work.
That matters in Plano. Many people looking for help here are trying to protect a job, keep family life stable, and get treatment for both substance use and mental health at the same time. A program that cannot handle that reality will fall apart under pressure.
Dual diagnosis care
Substance use rarely shows up alone.
A person may be drinking to stop panic before presentations, misusing pills to sleep, or using stimulants while anxiety, depression, trauma, or bipolar symptoms keep pushing everything off balance. If a center only treats the substance use, it leaves the main driver untouched.
Strong dual diagnosis care usually includes:
- Integrated treatment: The same clinical plan addresses mental health and addiction together.
- Psychiatric oversight when appropriate: Medication questions, symptom shifts, and side effects get timely attention.
- Therapists who understand co-occurring disorders: They look for patterns, not character flaws.
- Practical coordination: Treatment decisions make sense for real life, including work demands, family stress, and sleep disruption.
For professionals in the Dallas area, this is a screening issue. If the anxiety, trauma, or depression is not being treated with the addiction, keep looking.
Medication-assisted treatment
For opioid use disorder, medication-assisted treatment should be considered necessary when clinically appropriate. Families should ask about it early and ask plainly.
Medications such as buprenorphine lower withdrawal symptoms and cravings, which gives people a real chance to stay engaged in therapy and daily responsibilities. The Substance Abuse and Mental Health Services Administration describes medications for opioid use disorder as a proven part of treatment that supports recovery and reduces illicit opioid use. Programs that dismiss MAT on principle are showing you outdated clinical judgment.
Ask three direct questions:
- Does the program support MAT for opioid use disorder?
- Who manages those medications and monitors response?
- Is MAT integrated with therapy, or treated like a side issue?
If the answers are vague, take that seriously.
If cravings are driving relapse, treatment needs a medical response, not just encouragement.
Individualized treatment plans
Outpatient care only works when the plan fits the person’s actual week.
A Plano executive with alcohol misuse, panic symptoms, and late-night isolation needs a different structure than a younger adult with cannabis dependence, family conflict, and poor follow-through. One may need evening sessions, psychiatry, and relapse planning around travel or client dinners. The other may need tighter accountability, family work, and help rebuilding basic routine.
A strong treatment plan should answer specific questions:
- What problems are creating risk day to day?
- Which triggers are tied to work, relationships, trauma, or untreated psychiatric symptoms?
- What support exists at home, and what is missing?
- How will the team respond if attendance drops, substance use continues, or mental health worsens?
Families should expect the plan to change as the client changes. Static treatment plans usually mean generic care.
Evidence-based therapies
Clinical language gets used loosely in this field. Ask what happens in session.
Good outpatient programs use therapies with a clear method and a clear purpose. That often includes CBT, motivational interviewing, relapse prevention, trauma-informed therapy, and skills work focused on emotional regulation, communication, and coping under stress. Those approaches matter because they give clients tools they can use at 7 a.m. before work, after a triggering phone call, or on the drive home when the urge to use hits hard.
The right therapy should help clients:
- Catch distorted thinking before it turns into action
- Interrupt automatic substance use patterns
- Handle stress, conflict, and shame without using
- Communicate more openly with family, employers, and clinicians
- Recover faster after lapses instead of disappearing from care
A quick quality checklist
Before enrolling, a family should be able to confirm the basics without chasing vague answers:
| Standard | What to look for |
|---|---|
| Dual diagnosis | One treatment plan for both mental health and substance use |
| MAT access | Clear support for opioid recovery medications when appropriate |
| Individual planning | A schedule and clinical approach built around the person’s risks and responsibilities |
| Evidence-based therapy | Structured therapy with defined goals, not generic support groups alone |
These four pillars separate serious treatment from polished marketing. If a program is weak in any one of them, the gap usually shows up fast in attendance, engagement, relapse risk, or mental health instability.
Critical Questions to Ask Before You Enroll
A family in Plano often starts calling programs during a lunch break, after a bad weekend, or after one more promise to cut back falls apart. The pressure is real, and polished admissions language can make a weak program sound stronger than it is.
Ask sharper questions.
That matters even more for working professionals and people dealing with anxiety, depression, trauma, or burnout along with substance use. An outpatient program has to fit real life and treat the full clinical picture. If a center cannot explain how it handles both, keep looking.
Ask how the program makes treatment decisions
Start here. You need to know how the team decides whether someone belongs in PHP, IOP, or a different level of care.
A family should ask:
- Who completes the clinical assessment, and how soon does it happen?
- What factors determine the weekly schedule and level of care?
- How do you handle clients who need treatment but still have work obligations?
- How do you decide whether mental health symptoms need psychiatric support, higher structure, or a different setting?
Clear answers show clinical judgment. Vague answers usually mean the schedule is being sold before the person is being assessed.
Ask how progress is reviewed
Attendance is not enough. A serious program should be able to explain what improvement looks like and what triggers a change in the plan.
Ask these questions directly:
- How do you measure progress during treatment?
- How often is the treatment plan reviewed?
- What tells you that care is working, or not working?
- What happens if a client keeps missing groups, relapses, or stops engaging?
You are listening for specifics. The team should describe reassessment, schedule changes, therapist involvement, psychiatric review when needed, and a practical response to setbacks.
Ask what happens when the first plan fails
This question separates serious treatment from passive treatment.
Recovery rarely moves in a straight line, especially for professionals trying to protect a job while handling cravings, sleep problems, panic, depression, or relationship stress. A strong outpatient program should have a defined response when symptoms worsen or the structure is no longer enough.
Ask about:
- Clinical reassessment after relapse or rising cravings
- A step up from IOP to PHP when more support is needed
- Psychiatric follow-up if mood, trauma, or anxiety symptoms intensify
- Coordination with outside providers when the client already has a therapist, psychiatrist, or EAP contact
If the answer sounds like "we encourage them to try harder," move on.
Ask how family involvement actually works
Families do not need sales language about support. They need a clear role.
Use these questions:
- Are family sessions available, and who leads them?
- How do you help spouses, parents, or partners respond without enabling?
- What communication can families expect while privacy rules are still respected?
- How do you prepare the household for evenings, weekends, and discharge?
Home stress can keep a person stuck. Good treatment addresses it directly.
Red flags to take seriously
Some warning signs show up fast:
- The team avoids direct answers
- Everyone is described as a fit for the same schedule
- Work, parenting, or transportation concerns get brushed off
- Mental health symptoms are treated as secondary
- There is no clear plan for relapse, step-up care, or discharge support
Before you commit, review the program’s admissions process for outpatient rehab in Plano and compare what you read with what you hear on the phone. A strong center will answer questions clearly, explain its reasoning, and make the next step feel organized instead of pressured.
Your Path to Recovery Starts Here How to Get Started
It is 9:30 p.m. in Plano. A spouse is searching on a phone after another bad night, trying to figure out whether outpatient care can work with a job, a commute, and mental health symptoms that are getting worse. That family does not need a generic list. They need a clear next step.
Start with the call.
What happens on the first call
When someone calls (888) 385-2051, the job of admissions is straightforward. Find out what is happening, decide whether outpatient treatment is appropriate, and explain the next step clearly.
For working adults and people dealing with both addiction and mental health symptoms, that first conversation should cover the issues that affect success:
- What substances are involved and how recent the use is
- Whether anxiety, depression, trauma, panic, or mood swings are also part of the picture
- Whether the person is stable enough to be outside treatment hours
- How work, parenting, school, and transportation affect scheduling
- What insurance may cover and how fast an assessment can happen
If the call leaves a family more confused than before, keep looking. Good admissions teams bring order to a stressful situation.
What a strong admissions process should do
A strong process does more than collect insurance information. It should give you a recommendation you can act on.
The next step usually includes a clinical assessment and benefits review. Families can review the outpatient rehab admissions process in Plano before they call so they know what to expect.
Here is the standard to use:
| Question | What a strong process should provide |
|---|---|
| Is outpatient the right fit? | A clinical answer based on safety, symptoms, and stability |
| What level of care makes sense? | A direct recommendation for PHP, IOP, or another option |
| Can this work with a real schedule? | Practical guidance for work hours, family demands, and commuting in the DFW area |
| Will co-occurring disorders be addressed from the start? | A plan that includes mental health care, not a promise to deal with it later |
| What happens with insurance? | Clear verification, expected costs, and next steps |
Speed matters here. Once someone is ready for help, delays make it easier to back out, minimize the problem, or get pulled back into the same routine.
Ask about the first week, not just admission
Families often focus on getting in the door. Ask what happens immediately after that.
A good program should be able to explain how the first week is structured, how the schedule is built around actual responsibilities, and how progress is reviewed if the client is a professional trying to stay employed or a person whose depression, trauma, or anxiety is tied closely to substance use. If the answer is vague, the program is not organized enough.
You should also ask how the team handles changes fast. Some people need more support than expected once treatment starts. Others are stable enough for an evening IOP schedule that protects work and family responsibilities. A serious provider will explain how those decisions get made.
Bring up aftercare right away
Aftercare should be part of the first real conversation, not an afterthought at discharge.
Ask these questions early:
- How do you decide when someone should step down from PHP to IOP?
- What support continues after IOP ends?
- Are relapse prevention plans reviewed before discharge, not just handed over at the end?
- What follow-up support is available if work stress or mental health symptoms flare up again?
The best programs prepare clients for life after structured treatment while treatment is still underway. That matters even more for adults returning each day to demanding jobs, long commutes, family pressure, or home environments that can trigger relapse.
Someone who needs help today does not need to solve everything today. They need to make contact, get a clinical read on the situation, and choose the right level of care. Calling (888) 385-2051 is a practical first move. If substance use is hurting work, relationships, health, or stability, it is serious enough to address now.
Frequently Asked Questions About Rehab in Plano TX
Can someone keep a job while attending an IOP program
Often, yes. That’s one of the main reasons intensive outpatient care works well for working adults in the DFW area.
The key issue isn’t just time. It’s whether the person can participate consistently, stay safe outside sessions, and manage work stress without treatment becoming an afterthought. If job demands are intense, the program schedule needs to be realistic from the start.
Is outpatient treatment enough for serious addiction
Sometimes yes, sometimes no. The deciding factor is clinical stability.
If the person can remain safe outside treatment hours, has a workable home environment, and can engage consistently, outpatient treatment can be a strong fit. If withdrawal risks, medical concerns, severe relapse patterns, or dangerous instability are present, a higher level of care may be more appropriate first.
What if mental health is part of the problem
Then the program should address both issues together. Treating addiction without addressing anxiety, depression, trauma, or other mental health symptoms usually leads to weak results.
Families should look for dual diagnosis care, psychiatric support when appropriate, and therapists who understand how substance use and emotional distress reinforce each other.
Does family involvement matter
Yes. It often matters a lot.
Addiction changes trust, communication, finances, and daily routines. Family participation can help rebuild structure, improve boundaries, and reduce the chaos that often fuels relapse. The exact level of involvement depends on the client’s needs and privacy, but a strong program won’t ignore the family system.
What types of insurance are usually accepted
Coverage varies, so the only useful answer is a verified one. Many outpatient programs in the Dallas-Fort Worth area work with insurance and help families understand benefits before treatment begins.
The right next step is to verify benefits directly instead of guessing based on a website. That prevents surprises and helps the family understand what level of care is financially realistic.
How long does treatment last
There is no honest one-size-fits-all timeline. Length depends on symptom severity, substance history, mental health needs, attendance, response to treatment, and relapse risk.
A trustworthy provider should explain how progress is reviewed and how decisions are made about stepping down or extending care. Programs should adapt to the person, not force the person into an arbitrary finish line.
What should a family do today if they’re overwhelmed
They should narrow the task. Don’t try to master the whole treatment system in one night.
A practical sequence is better:
- Call and describe the situation accurately.
- Ask which level of care appears appropriate.
- Verify insurance and scheduling.
- Ask about dual diagnosis, MAT, and aftercare.
- Move quickly if the fit is right.
Waiting for certainty keeps a lot of families stuck. Clarity usually comes after contact, not before it.
Maverick Behavioral Health helps adults in Euless, Dallas, Plano, and the greater DFW area find structured outpatient treatment that fits real life. The program offers PHP, IOP, standard outpatient care, dual diagnosis treatment, and MAT support in a private setting built for recovery with dignity. To speak with a compassionate admissions team, call (888) 385-2051. A confidential conversation can clarify the right level of care, verify insurance, and help a family take the next step without delay.