TL;DR: The typical intensive outpatient program cost is $3,000 to $10,000 for a treatment episode, and daily rates in the Dallas-Fort Worth area often fall between $250 and $350 before insurance. Many PPO plans can reduce what a person pays out of pocket, which is why insurance verification should happen before admission.
The search usually starts the same way. Someone in Dallas, Euless, or somewhere else in DFW knows help is needed, but one question keeps stalling the next step: “How much is this going to cost?”
That concern is reasonable. Treatment is a health decision, but it’s also a financial decision. People still have rent, car payments, children, work schedules, and classes. A good answer has to cover more than a broad price range. It has to explain what’s included, what changes the price, how insurance works, and what to ask before committing.
Table of Contents
- Understanding the True Cost of an Intensive Outpatient Program
- Key Factors That Influence Your Final IOP Price
- Comparing IOP Costs to PHP and Inpatient Rehab
- How Insurance Covers IOP Treatment in the Dallas Area
- Estimated IOP Costs in Dallas-Fort Worth and Euless
- Your Checklist for Discussing IOP Costs and Payments
- Take the Next Step Toward Affordable Recovery Today
Understanding the True Cost of an Intensive Outpatient Program
A common DFW scenario looks like this: an adult knows alcohol or drug use is getting harder to manage, but stopping work for residential treatment doesn’t feel possible. That person needs structured care, but also needs to keep showing up for life.
That’s where an intensive outpatient program often fits. The average intensive outpatient program cost for substance use treatment ranges from $3,000 to $10,000 per episode or month, with daily rates typically around $250 to $350. By comparison, inpatient rehab can run $10,000 to $60,000 monthly, which makes IOP 50-80% more cost-effective while allowing clients to keep working and stay connected to family life, according to this breakdown of intensive outpatient program cost ranges.
What the base price usually includes
People often see a quote and assume they’re paying for “just group.” That’s usually not how a real IOP works.
A standard program generally bundles several services into one level of care. That commonly includes group therapy, individual counseling, psychiatric support when needed, medication management, relapse prevention work, and treatment planning. Some programs also include family involvement and support for co-occurring mental health needs.
For many adults, that package matters more than the top-line number. A lower quote isn’t always a better value if it leaves out key pieces of care that reduce setbacks later.
A helpful starting point is understanding what IOP therapy involves in practice. Once that’s clear, price comparisons become more realistic.
Practical rule: The real question isn’t only “What does IOP cost?” It’s “What care is included in that cost, and does it match the person’s clinical needs?”
Why many adults choose IOP over residential care
An IOP asks for a serious commitment, but it doesn’t require putting life on hold in the same way inpatient treatment does. That trade-off matters for professionals, parents, and students across Dallas-Fort Worth.
The value isn’t just the lower program fee. It’s also the ability to avoid some hidden costs tied to leaving work, pausing school, or stepping away from family responsibilities.
That doesn’t mean IOP is the right fit for everyone. Some people need a higher level of care. But for adults who are safe to receive treatment without a residential stay, IOP often gives a strong middle ground: more structure than standard outpatient therapy, and more flexibility than inpatient treatment.
Key Factors That Influence Your Final IOP Price
Two people can both be told they need IOP and still receive very different cost estimates. That isn’t automatically a red flag. It usually means the programs aren’t built the same way.
Intensity and schedule shape the quote
An IOP isn’t a flat product. It’s closer to a treatment framework with a range of schedules inside it.
Daily IOP rates can range from $250 to $650, reflecting ASAM Level 2.1 care standards. Programs become more expensive as the weekly schedule becomes more intensive and the treatment plan includes more services. That same source notes that therapies such as CBT or EMDR can increase expenses by 15-25% each because they require specialized staffing, and enhanced IOPs with case management have shown 40% lower readmission rates than standard outpatient care, according to this explanation of IOP pricing variables and enhanced services.
A shorter weekly schedule may cost less up front. It may also provide less support. That’s the trade-off.
A more robust schedule can make sense when someone is stepping down from a higher level of care, managing repeated relapse, or trying to stabilize both substance use and mental health symptoms at the same time.
Specialized services raise cost and often raise value
Specialized care tends to push pricing toward the higher end. That includes:
- Medication-assisted treatment: MAT adds medical oversight, medication management, and follow-up.
- Dual diagnosis care: Treating substance use alongside depression, anxiety, trauma, or another mental health condition usually requires more coordination.
- Case management: This helps with practical barriers such as work notes, outside referrals, scheduling, and aftercare planning.
- Family services: Bringing family into treatment can improve alignment at home, but it also adds clinician time.
The important point isn’t that “more services” always means better care. It means the plan should match the actual problem.
Treatment gets expensive when people pay for the wrong level of care, or for a program that leaves out the support they clearly need.
Location and staffing matter in DFW
Dallas-Fort Worth is a major metro area. That affects pricing.
Urban markets often carry higher operating costs, and programs that use licensed clinicians, psychiatric support, and structured specialty tracks may price higher than bare-bones options. Sometimes that extra cost reflects better access to services a person would otherwise need to arrange separately.
A useful way to think about the quote is this:
| Cost driver | What it changes |
|---|---|
| Weekly hours | More clinical time raises program cost |
| Program length | Longer treatment usually means a higher total fee |
| MAT or psychiatric support | Adds medical oversight and follow-up |
| Dual diagnosis focus | Requires broader clinical coordination |
| Family and case management services | Expands support beyond therapy sessions |
| DFW market location | Can increase baseline pricing |
Low price alone doesn’t prove efficiency. High price alone doesn’t prove quality. The key is whether the treatment plan is clinically appropriate and financially clear.
Comparing IOP Costs to PHP and Inpatient Rehab
Cost only makes sense when it’s tied to the level of care. A person choosing between IOP, PHP, and inpatient treatment isn’t really choosing between three prices. That person is choosing between three different structures of daily life and clinical support.
A side by side view of the trade-offs
For adults in Dallas-Fort Worth with co-occurring disorders, choosing between IOP and PHP is both a clinical and financial decision. Evidence suggests that matching treatment intensity to actual clinical need can reduce total healthcare costs by 25-35% by preventing relapse and crisis utilization, as described in this discussion of IOP, PHP, and long-term cost effectiveness.
That principle matters. If a person needs more support than IOP can safely provide, choosing IOP because it’s cheaper may lead to instability. If a person is stable enough for IOP but enters a heavier level of care than necessary, the added expense may not improve results.
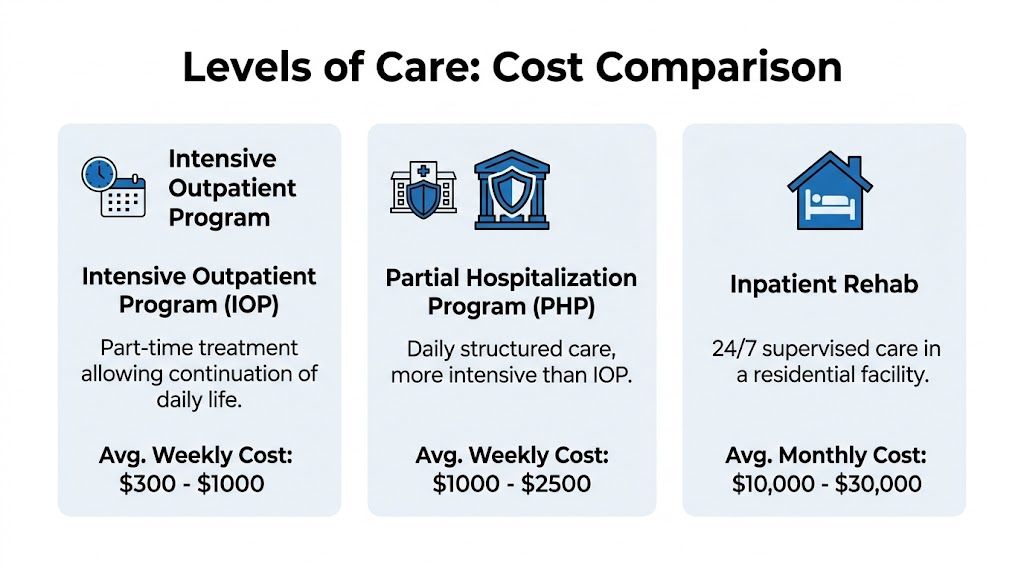
| Feature | Intensive Outpatient (IOP) | Partial Hospitalization (PHP) | Inpatient/Residential |
|---|---|---|---|
| Living at home | Yes | Usually yes | No |
| Schedule intensity | Part-time, structured | More hours and more clinical structure | Full-time with 24/7 support |
| Best fit | People who need significant support but can still function outside treatment | People who need near-daily structured treatment without overnight stay | People who need round-the-clock supervision |
| Work or school flexibility | Often possible with planning | Usually limited | Generally paused |
| Cost pattern | Mid-range outpatient cost | Higher than IOP in many cases | Highest overall cost |
The right level of care protects both recovery and budget
A working adult in Euless may do very well in IOP if the person can remain safe between sessions, attend consistently, and use outside supports. A different adult with severe instability, repeated crises, or a difficult withdrawal picture may need PHP or inpatient care first.
That’s why the cheapest option isn’t always the least expensive in the long run.
A good admissions process doesn’t sell a program. It identifies the minimum effective level of care that still protects safety and progress.
IOP often offers the best return when someone needs meaningful structure but also needs to keep practicing recovery in real life. PHP can make more sense when someone needs closer monitoring during the day. Inpatient rehab is often necessary when the home environment, withdrawal risk, or symptom severity makes outpatient care unsafe.
How Insurance Covers IOP Treatment in the Dallas Area
Patients typically do not pay the full sticker price for IOP. Insurance changes the actual number, sometimes dramatically. The problem is that many people don’t know how to verify benefits correctly, and that uncertainty can delay care.
The terms that change what you actually pay
A few insurance terms have an outsized effect on the final bill:
- PPO: Usually gives more flexibility in choosing providers. Out-of-pocket costs still depend on network status, deductible, and coinsurance.
- HMO: Often requires tighter network use and may involve more referral rules.
- In-network: The provider has a contracted rate with the insurer. This is usually where costs are more predictable.
- Out-of-network: The provider doesn’t have that contracted rate. The plan may still pay something, but the member’s share can rise quickly.
- Deductible: What the member may need to pay before fuller insurance benefits begin.
- Coinsurance or copay: The portion the member pays after insurance processes the claim.
- Preauthorization: Approval some plans require before treatment starts.
People often assume “covered” means cheap. It doesn’t. It only means the plan may contribute under certain rules.
A person can get a useful overview of how outpatient rehab services are covered by insurance before calling, but the actual benefits still have to be checked against the specific plan.
A practical insurance verification checklist for the phone call
When calling an admissions team or insurer, the most useful questions are direct:
Ask whether IOP is an in-network benefit.
If the answer is unclear, that uncertainty should be resolved before scheduling.Ask whether preauthorization is required.
If it is, find out who submits it and what documents are needed.Ask about the deductible status.
A plan may cover IOP, but the member may still owe more early in treatment if the deductible hasn’t been met.Ask how the plan handles dual diagnosis and psychiatric services.
Some parts of care may process differently than basic therapy services.Ask for an estimate of the member responsibility per session or per day.
That’s often more practical than asking only for a broad percentage.Ask whether out-of-network benefits apply if in-network placement isn’t available.
This matters when timing is urgent and local options are limited.
One practical option in the DFW market is having a treatment center verify benefits directly. Maverick Behavioral Health accepts many PPO plans and helps prospective clients confirm coverage and expected out-of-pocket responsibility before admission.
Why delays and out of network placement get expensive fast
Insurance problems don’t just create paperwork headaches. They can change whether treatment starts at all.
Industry data suggests 30-40% of initial IOP admissions face 3-7 day delays because of incomplete insurance verification. For DFW patients, out-of-network placement can increase out-of-pocket costs by 40-60%, which may amount to a $3,750 monthly difference in some scenarios, according to this analysis of insurance verification delays and out-of-network cost impact.
That’s why waiting until the day of admission to sort out benefits usually doesn’t work well.
“Can you verify my IOP benefits, confirm network status, and give me a written estimate of what I may owe?” That single question can prevent a surprising amount of stress.
A fast admission is helpful only if the financial details are accurate. Clean verification protects both access and trust.
Estimated IOP Costs in Dallas-Fort Worth and Euless
People looking for treatment close to home usually want more than a national average. They want a local range they can use for planning.
What local pricing often looks like
In Texas, the average daily cost for an Intensive Outpatient Program without insurance ranges from $250 to $350. For a typical program operating 3 days a week, that works out to about $3,000 to $4,200 per month before insurance, and verifying a PPO plan can often reduce out-of-pocket costs to $50 to $100 per session, according to this Texas-focused IOP cost guide.
For someone living in Euless, Arlington, Dallas, Fort Worth, or nearby communities, that range is usually more useful than a generic national estimate because it reflects what treatment shopping feels like in this part of Texas.
Some programs will sit near the lower end because they offer a simpler structure. Others will sit higher because they include broader clinical services or more frequent treatment days.
A local option can also reduce practical strain. Less driving across the metroplex can make attendance easier, especially for adults balancing work, family, and court, school, or medical appointments. For those comparing nearby options, this intensive outpatient program in Euless, Tarrant County, Texas gives a concrete picture of what local outpatient care can look like.
Why local access can lower total treatment strain
The posted program fee is only part of affordability. Commuting time, missed work hours, and scheduling friction affect whether someone can stay engaged long enough to benefit.
That’s especially true in DFW, where distance alone can turn a realistic treatment plan into an exhausting one. A program that fits the person’s daily route and schedule may be easier to complete, even if the headline price isn’t the absolute lowest option found online.
Your Checklist for Discussing IOP Costs and Payments
Many people feel more anxious about the financial call than the clinical one. A short checklist gives the conversation structure and keeps important questions from getting missed.
Questions worth asking before admission
Bring these questions to any admissions call:
- What is the full estimated cost of care? Ask for the expected total, not just the daily or session rate.
- What services are included in that quote? Clarify whether the estimate includes individual therapy, group sessions, psychiatric visits, medication management, family work, and discharge planning.
- What isn’t included? This question often reveals separate charges or outside referrals.
- Has insurance already been verified? If yes, ask whether the estimate is based on confirmed benefits or only a preliminary guess.
- Is the program in network with the plan? If not, ask how out-of-network claims are handled and what the likely member responsibility may be.
- Will preauthorization be required? If it is, ask who manages that process and whether admission must wait for approval.
- How are missed sessions handled financially? Attendance policies matter.
- Is there a written estimate? Verbal quotes are helpful, but written estimates reduce confusion.
- Are payment arrangements available if the out-of-pocket share is still hard to manage? It’s better to discuss this before treatment begins than after bills arrive.
A prepared caller usually gets clearer answers. Clear answers make it easier to commit to care with less fear and less second-guessing.
The best financial conversation is the one that happens before admission, not after the first claim is processed.
Take the Next Step Toward Affordable Recovery Today
Cost matters. It should. But uncertainty about cost shouldn’t keep someone stuck when treatment may already be overdue.
An intensive outpatient program can offer meaningful clinical support without the financial and logistical weight of residential care. The key is getting specific answers about level of care, insurance, network status, and what the quoted fee really includes.
For adults in Dallas, Euless, and the wider DFW area, the most useful next step is simple: ask for a benefits check and a clear estimate before making a decision. That turns treatment from a vague expense into a concrete plan.
Anyone who wants help understanding options, verifying insurance, or discussing IOP affordability can call (888) 385-2051 for a confidential conversation.
Maverick Behavioral Health helps adults in Euless and across Dallas-Fort Worth explore outpatient treatment options, verify insurance, and understand the practical cost of care before admission. Call (888) 385-2051 to speak with the admissions team and get clear next steps.